Introduction
Antibiotic resistance has become a major concern in the field of medicine, as it poses a significant challenge to global public health. The effectiveness of antibiotics in treating bacterial infections has played a crucial role in modern medicine, saving countless lives. However, as the prevalence of antibiotic resistance increases, the urgent need for the development of new drugs becomes more apparent. This article delves into the complexities of creating new antibiotics to combat resistance, exploring the evolving landscape of medicine development in the face of bacterial pitfalls.
The Rising Antibiotic Resistance Crisis
Antibiotic resistance occurs when bacteria evolve mechanisms to repel the goods of medicines designed to exclude them. The Centers for Disease Control and Prevention( CDC) estimates that at least 2.8 million people in the United States acquire antibiotic-resistant infections each time, resulting in over 35,000 deaths.
The overuse and abuse of antibiotics in both humans and creatures contribute significantly to the development of resistance. As a result, there’s a critical need for new antibiotics with innovative mechanisms of action.
Challenges In Antibiotic Drug Development
1. Profitable Viability
Developing new antibiotics is a financially parlous bid for pharmaceutical companies. Unlike chronic specifics that cases may take for extended ages, antibiotics are frequently specified for short durations. This limits the implicit request size and profit compared to medicines for habitual conditions. The profitable challenges discourage investment in antibiotic exploration and development.
Statistics According to a report by the Pew Charitable Trusts, only a sprinkle of major pharmaceutical companies are laboriously engaged in antibiotic exploration.
2. Regulatory Hurdles
The number of major drug companies engaged in the development of antibiotics shrank significantly between the years 2009 and 2018, from 18 to 12.
strict nonsupervisory conditions for antibiotic blessing can hamper the development process. The need for expansive clinical trials to demonstrate safety and efficacity is essential but time-consuming. Streamlining nonsupervisory pathways for antibiotics without compromising safety norms is a delicate balance that the assiduity and nonsupervisory bodies must navigate.
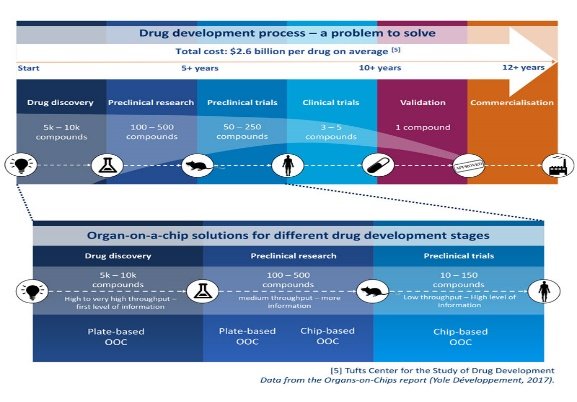
Statistics A study published in Clinical Infectious Conditions set that, on average, it takes over a decade for a new antibiotic to progress from the preclinical stage to blessing. also, the success rate for antibiotics in clinical development is lower than for other remedial areas, making it a parlous investment
3. Scientific Complexity
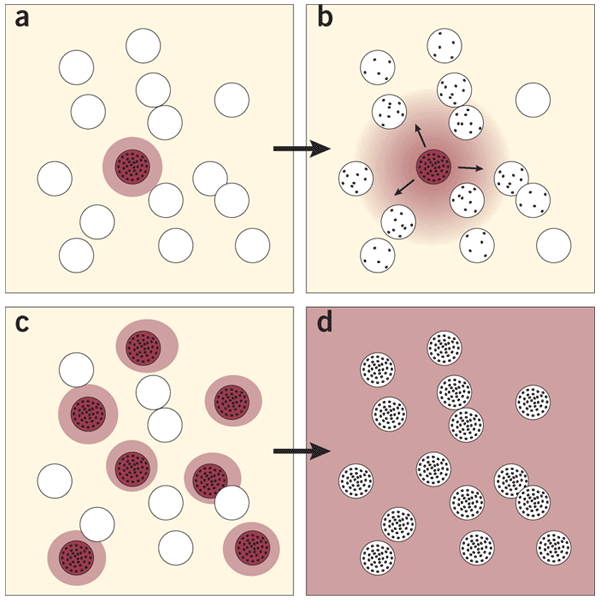
The discovery of new antibiotics is complicated by the vast diversity of bacteria and their capability to acclimatize fleetly. relating new composites that widely target bacteria without harming mortal cells is a complex scientific challenge. The intricate biology of bacteria and the eventuality of resistance mechanisms to crop during medicine development further complicate the process.
4.Market Dynamics
The pharmaceutical request’s focus on blockbuster medicines for habitual conditions has led to a relative neglect of antibiotic development. The limited request eventuality for antibiotics makes it less seductive for large pharmaceutical companies, contributing to a lack of investment in this critical area.
5.Rapid Emergence Of Resistance
As new antibiotics are introduced, bacteria can snappily develop resistance. This rapid-fire elaboration underscores the significance of ongoing exploration and development to stay ahead of arising resistant strains
Advancements In Antibiotic Research
1. Targeting Novel Bacterial Mechanisms
In recent times, experimenters have concentrated on relating new bacterial targets that differ from those of antibiotics. This involves understanding unique bacterial processes that can be exploited without harming mortal cells. For illustration, experimenters are probing the eventuality of dismembering bacterial biofilms, which are defensive layers that make bacteria resistant to antibiotics.
2.Precision Medicine
Advancements in genomics and individualized drugs offer new openings for targeted antibiotic remedies. By understanding the inheritable makeup of both the pathogen and the case, experimenters can develop acclimatized treatments that are more effective and less prone to resistance.
Statistics A study in Nature Dispatches reported successful issues in cases with cystic fibrosis using substantiated antibiotic combinations grounded on individual microbial biographies. This approach redounded bettered clinical issues and reduced antibiotic resistance.
3. Combination Curatives
Combining multiple antibiotics or combining antibiotics with antibiotic medicines is gaining attention as a strategy to overcome resistance. The combination approach aims to target bacteria through multiple mechanisms, making it harder for them to develop resistance. This approach has shown a pledge in preclinical studies, and some combination curatives are formerly in clinical trials.

4. Harnessing Technology
Advancements in technology, similar to artificial intelligence and high-outturn webbing, are accelerating the medicine discovery process. Machine literacy algorithms can dissect vast datasets to prognosticate implicit medicine campaigners, significantly reducing the time and coffers needed for early-stage medicine development. High-outturn webbing allows experimenters to test thousands of composites snappily, relating implicit antibiotics more efficiently.
5.Novel Drug Delivery Systems
Innovative medicine delivery systems, including nanoparticles and controlled-release phrasings, can ameliorate the pharmacokinetics of antibiotics, leading to better case compliance and enhanced remedial issues.
6.Synthetic Biology And CRISPR
The arrival of synthetic biology and CRISPR technologies allows experimenters to wangle bacteria-killing motes and modify antibiotics to overcome resistance mechanisms. This approach offers an important tool for staying ahead of evolving bacterial pitfalls.
7.Global Collaboration And Hookups
Feting the global nature of antibiotic resistance, cooperative sweat among governments, pharmaceutical companies, academia, and nonprofit associations is pivotal. enterprise similar to the Global Antibiotic Research and Development Partnership( GARDP) aims to address the lack of investment and promote exploration in this field.
8.Indispensable Curatives
Experimenters are exploring indispensable approaches to traditional antibiotics, similar to bacteriophage remedy, which utilizes contagions that infect and kill bacteria.
Statistics A clinical trial published in The Lancet Infectious Conditions demonstrated the efficacity of phage remedy in treating antibiotic-resistant infections, with a success rate of over 80 in cases with habitual bacterial infections.
Global Enterprise To Encourage Antibiotic Development
Feting the critical need for new antibiotics, colorful global enterprise aims to incentivize exploration and development in this field.
1. Request- Grounded Impulses
Governments and transnational associations are exploring request-grounded impulses to encourage pharmaceutical companies to invest in antibiotic exploration. These impulses may include a guaranteed request, extended exclusivity ages, or other fiscal prices for successful antibiotic development.
2. Public-Private Hookups
Collaborations between governments, academia, and the private sector are becoming increasingly common. These hookups work the strengths of each sector, combining coffers and moxie to accelerate antibiotic exploration. The Combating Antibiotic-Resistant Bacteria Accelerator( CARB- X) is one similar action that supports beforehand- stage development of innovative antibacterial products.
3. Prize Finances And Awards
Prize finances and awards are designed for award-successful antibiotic development rather than counting solely on traditional request impulses. Thesenon-traditional models aim to link fiscal returns from the volume of antibiotic deals, ensuring that successful medicines are awarded grounded on their societal impact.
Conclusion
The future of antibiotics depends on our capability to overcome the challenges associated with antibiotic resistance and medicine development. While the hurdles are significant, advancements in wisdom, technology, and global enterprise give a stopgap for the development of new and effective antibiotics.
By addressing profitable walls, streamlining nonsupervisory processes, and fostering collaborations, the global community can work together to ensure a robust channel of antibiotics to guard public health in the face of evolving bacterial pitfalls.
The urgency of this task can not be exaggerated, and combined sweats are needed to secure a future where antibiotics remain a foundation of ultramodern drugs.